Keziah Shorten was a 19-year old teenager from England and officially Paolo Macchiarini 3rd patient receiving a cadaveric trachea transplant. She suffered from a slow growing form of cancer and received a cadaveric trachea transplant from Macchiarini at the Careggi hospital in Florence. After life-threatening complications ensued, her second transplant, a plastic trachea made and implanted at UCL and its UCL hospital (UCLH) in London, failed also. Keziah died one and a half years after her first operation. With new evidence provided to me by a source close to the patient, I present here a version of Keziah’s story which is very much different from the official one. This makes UCL and UCLH at least in part responsible for her death, from the very beginning. It was their decision to treat Keziah with the first cadaveric transplant, which sealed her fate. Next to the UCL honorary professor Macchiarini himself, the British doctors, who according to my source promised Keziah a complete cure and initiated this transplant, were UCL professors and surgeons Martin Birchall and Paul O’Flynn. Keziah was even supposed to be operated at UCLH, but once Macchiarini got an ethics permit in Italy, she was moved there. O’Flynn followed her and joined Macchiarini in the transplant operation. Afterwards, it was an ongoing catastrophe which was exacerbated by an apparent botched intervention at UCL Hospital. Death seemed a relief after terrible suffering imposed on Keziah by fame-seeking doctors worshipping their own magic of regenerative medicine.
Macchiarini was recently acquitted by Italian tribunal of all charges of extortion and fraud, originally raised against him in 2012 which even led to a house arrest. The issue here was his referring of terminally ill patients to hospitals in UK and Germany for a promise of cure and the hefty costs thereof. Macchiarini’s trachea transplants at the Florentine hospital Careggi between 2010 and 2011 are not even being investigated by the Italian justice. Noone seems to be interested in their deaths. One of these victims was Keziah.
I previously wrote about Keziah’s trachea transplant and first evidence of the suspected role of UCL in this article. Recently, I was approached by a witness (identity known to me) who gave me all the information which UCL Hospital still refuses to release by calling my request “vexatious”. Another source of the information was an account of Keziah’s suffering written by her father on internet, which that witness confirmed to me as being correct. The following is therefore very much different from the official version of Keziah’s story, postulated by Birchall. Because everyone responsible keeps silent (even the UCL and UCLH press offices refused to comment), I do not have the “official” evidence. But it certainly exists, and an external investigative commission, tasked by UCL to look into the deeds of Macchiarini and Birchall in London, should have no trouble getting that evidence. Let’s hope they make it public and put it to good use.
Official version
Here is the version of Keziah’s story by Birchall and his coauthors, published in Culme-Seymour et al 2015:
“This patient was a 19-year-old woman with adenoid cystic carcinoma of the trachea, who had two separate transplants. The first transplant was a decellularized donor trachea, re-cellularized with autologous stem cells, and transplanted into the patient in Italy. The patient then travelled to UCLH for postsurgery care. Infection, likely exacerbated by the side effects of radiotherapy, caused a breakdown of the first transplanted trachea.
A second transplant was performed at UCLH 15 months after the first, with a synthetic trachea seeded with autologous stem cells at the UCL Biobank. Surgery was performed using the existing UK compassionate use legislation and with fully informed written consent. Sadly, the patient died 6 months after the second transplant due to mediastinitis, secondary to an esophageal fistula that is believed to have been unrelated to the transplant.
However, in the interim, she had 3 months at home with a good quality of life before her death. This is probably the first reported case of a complex tissue-engineered construct being deployed from the outset as a purely palliative surgical intervention”.
As you can read below, there was no good quality of life, just pain and suffering. As my source informed me, there was apparently even no infection, certainly not one introduced in Italy. The radiation therapy was discussed by Birchall and others already at UCLH, and left to be performed at Macchiarini’s discretion. The fistula (hole) in the oesophagus was actually directly related to the tracheal transplant, primarily Macchiarini’s radiation therapy which damaged the patient’s gullet and made much worse by a botched intervention at UCLH. The patient’s death was directly caused by the experimental two trachea transplants, both of which were done with direct involvement of UCLH doctors.

UCL’s false promise of cure
This is what Keziah’s father, Andy Kenyon, wrote on the JustGiving charity website:
“Kez had adenoid cystic carcinoma, growths in her trachea that was closing off her windpipe. Surgery was proposed where a section of the trachea would be removed, the thyroid gland removed, and because the tumours were also pressing into the oesophagus, a large section of the oesophagus would be cut out and her stomach would be brought up into her neck and be attached to what remained of the oesophagus.
Unfortunately all of her trachea was affected so sectioning the trachea was not an option so she chose pioneering stem cell surgery instead where a donor trachea would be transplanted. […] The stem cell approached had only been tried twice before and the operation took place in Florence Italy in July 2010”.
The latter information was a lie. Only the very first patient Claudia Castillo (whose situation already deteriorated seriously at that time, but was kept secret, see this report) and the freshly operated 10-year old Ciaran Lynch were mentioned to Keziah and her family. Macchiarini however operated in 2009 another Barcelona patient with a cadaveric trachea transplant, who then disappeared as if she never existed. The case of that middle-aged woman was even presented by Macchiarini when he and his partner Martin Elliott gave a talk about their patient Ciaran (see this article for details).
Keziah visited her family doctor toward the end of 2009, her only symptom was breathlessness. She was then referred to her regional area cancer centre, Guy’s and St Thomas’ hospital in London and diagnosed there in April 2010 after a bronchoscopy with adenoid cell carcinoma (ACC), a lethal, but very slow growing form of cancer (I described the disease here). Because of the nature of this disease, the hospital could not offer her a cure, only a more or less radical surgery. The entire cancer could not be removed without leaving her without a trachea. Hence, a partial trachea resection was proposed at Guy’s and St Thomas’ hospital, together with a tracheostomy (a breathing hole in throat, which makes speech difficult and puts some restriction onto the daily life). Some of the cancer-affected airway was suggested to be left in place, as it was estimated not to present any danger in the near future.
This is where Macchiarini and his UCL colleagues came into the picture. The famous surgeon was approached by members of Keziah’s family end of May 2010, because of his two alleged miracle cures which made world news. Already on July 13th 2010, Keziah was operated by him and the UCL surgeon O’Flynn in Florence. Why did Keziah agree to this?
When Keziah and her family met Macchiarini at his hotel in London in the end of May 2010, they were told how lucky she was to have met him at that time. The star surgeon made big promises about the success of the new field of stem cell transplants and how it was about to take off. Macchiarini then arranged for O’Flynn to repeat the diagnostics tests previously performed at the Guy’s and St Thomas’ hospital. O’Flynn phoned Keziah’s family at their home several times to set up the tests, which began in June 2010; many phone calls were exchanged between the family and the two surgeons. After the tests were completed, the family met Macchiarini and O’Flynn several times at UCHL to set up the operation. Keziah was scheduled to receive a cadaveric trachea transplant in London. Birchall was perceived by the family as “the boss” of all this. At all times, Keziah was promised by Macchiarini and O’Flynn that they would cure her, that it would be a very tough and demanding operation, but that she would be cured at the end. No more cancer, thanks to a cadaveric trachea and stem cell magic. The only time Keziah was told it may turn out differently was the day before her transplant in Florence took place. There, Macchiarini finally cautioned her that the operation may not be a complete success.
London cancelled, operated in Florence
Birchall’s official version is that he and his UCL had absolutely nothing to do with the first transplant Keziah received from Macchiarini in Florence. With the evidence I presented above, Birchall’s claim goes out of the window. But why was the operation moved to Careggi hospital in Florence in the first place, where Macchiarini had his main base at that time? And where was the donor graft prepared?
Birchall was already previously working together with Mark Lowdell and his lab at the Royal Free Hospital, where decellurised donor tracheas for patient transplants in London were prepared. One was made and delivered in March 2010 to be implanted into Ciaran. The official version, postulated by their partner the Great Ormond Street Hospital surgeon Martin Elliott, actually states that Macchiarini prepared that graft in Florence and had it delivered to UK. But as the Royal Free Hospital informed me (see update here) that this organ was made by Lowdell’s lab, just as Keziah’s second plastic trachea as well as Birchall’s and Elliott’s last (and horribly disastrous) trachea transplant for 15 year-old Shauna Davison in 2012 (most recently published as Elliott et al 2017). About Keziah’s first transplant however, Royal Free declared to me to hold no such records. Indeed, the evidence suggests it was made in Italy after all, but not for Keziah. It was apparently a decellurised organ Macchiarini already had “in stock”.
According to these official documents I made available before, Macchiarini submitted a request to the Italian National Transplant Centre (CNT) to harvest and decellurise human donor tracheas. Permission was granted on January 26th 2010. The documentation also suggests that an ethics council was appointed by the director of Careggi hospital on April 22nd 2010, to process Macchairini’s requests to operate patients with these grafts. At that time however, Macchiarini never even heard of Keziah yet, her family only contacted him in May 2010.
On June 14th, the Careggi ethics council met in an urgent meeting and approved Macchiarini’s request to transplant two patients with cadaveric tracheas. Right afterwards, Macchiarini informed Keziah’s family about the change of plans: the operation was to take place not at UCLH in London anymore, but at Careggi in Florence. At that time, Keziah was probably still being tested at UCL by O’Flynn. Did Macchiarini request an urgent ethics council meeting before those tests were complete? Was it actually possible to organize an ethics council with 16 participants on a few days’ notice? Can it be that Macchiarini submitted his request to save two patients before he even met Keziah?
This is how Alessandro Nanni Costa, head of the CNT described the background of this ethics vote:
“The referenced patient, affected by primitive adenoid cystic carcinoma of the trachea has been treated with the transplant of a donor’s trachea after a clinical assessment performed by the Guy’s & St. Thomas Hospital, Head and Neck Centre at the University College London Hospital and by a multidisciplinary clinical and oncological team at the Careggi Hospital in Florence. The experts that have evaluated the patient’s conditions have proposed the surgical resection with transplant as the therapeutic treatment. The other traditional therapeutic options that were considered, namely the surgical treatment (total laryngectomy, partial pharyngectomy, total esophagectomy with gastric pull-up), have been considered not appropriate”.
Guy’s and St. Thomas hospital sure never recommended any tracheal transplant. How Careggi experts could have evaluated Keziah’s medical state in early June 2010 is unclear. She never was in this Florentine hospital until the operation in July 2010. The ethics board obviously decided to operate Keziah with a cadaveric transplant based solely on the recommendations from Macchiarini and UCLH. After all, the British NHS was apparently paying, as I learned.
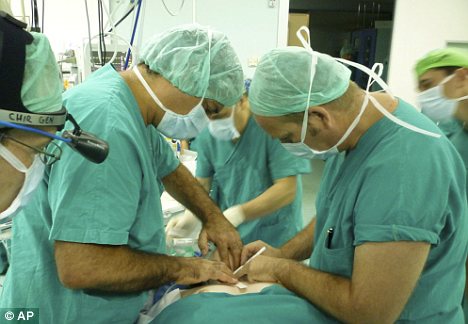
O’Flynn travelled to Florence (he is even seen on this photograph) and joined Macchiarini in the Careggi operation room to transplant Keziah with a decellurised organ which Macchiarini apparently already had “in stock”. Did it fit Keziah at all, and in which condition was it? We do not know. There was obviously no time between ethics vote and operation to prepare a custom-made trachea graft, since one needs time to find a suitable freshly deceased donor, with the following decellurisation process taking around 6 weeks (as explained in Macchiarini et al 2008). Unlike with Claudia Castillo, no bioreactor was used this time, as described in this newspaper article. Macchiarini started to apply already on his two previous patients a bizarre “bionic” method I described here, where bone marrow cells and growth factors are freshly dumped onto the graft during the operation.
Here is the consent form, a version of which Keziah signed. One cannot call it “informed consent” though, even if it was approved by Careggi ethics council. E.g. the claim that the growth factors, especially erythropoietin, have “no known side effects”, was a lie. Just like the one that Keziah’s predecessor Claudia Castillo had an “excellent quality of life”.
Right after Keziah, another woman, 31 year old young mother from Czech Republic, was transplanted by Macchiarini at Careggi, based on same ethics vote from June 14th 2010. She died upon return to her home country (see this Corriere Fiorentino report). Three more patients followed at Careggi, two died, one suffered irreparable brain damage.
Failed transplant and UCL’s wishful thinking
When Keziah returned to London, O’Flynn examined her and proclaimed to her family that the graft developed its own independent blood supply. Either O’Flynn saw a biological miracle, or he looked at the patient’s own remaining native trachea, or he simply made things up, but fact remains no other trachea recipient experienced any vascularisation of the decellurised cadaveric graft. Only formation of scar tissue and mucus.
Andy Kenyon describes in his post what happened to his daughter after the operation at Careggi:
“After 16 hours in surgery and 53 personel, Kez spent 2 long and painful weeks recovering, fighting for her life on more than one occassion, not being able to eat or drink for the first few days and having to cough regularly to remove the mucus build up in her lungs which after she had been cut open from neck to belly button was excruciatingly painful.
After her return to London [on July 30th 2010, -LS], she spent another week in hospital at University College Hospital in London before being released pending numerous returns to change her stent in her new trachea. The stent was keeping trachea open until the tissue around it grew back and supported it. She was in and out of hospital every month for about a week at a time recovering from these changes but she could eat and drink. […]
Finally the stent was removed in december 2010 but kez trachea closed due to swelling and a hole was discovered between her oesophagus and trachea. Emergency surgery got her intubated and she was put on life support for 2 weeks to allow the swelling in the trachea to go down. Unfortunately during this time the tube supplying her oxygen was yanked out and in haste to put it back in, the tube caught on the hole between the trachea and oesophagus a ripped it until it was 4 cm long. The oesophageal tissue was old and fragile because of the irradiation treatment during the italian operation and ripped easily.
Over christmas, She was slowly brought off life support and an operation was tried to repair the hole. This operation included fitting a tracheostomy as a temporary measure to take the strain off the effected area. The night after the operation the stitches ripped and kez almost died and had to fight for her life for a second time. But she recovered and went home for 3 weeks learning to cope with the tracheostomy. She could still eat, drink and talk at this stage.
In February 2011, A second attempt to close the hole resulted in the same thing happening, the stitches ripped, breathing became a problem, in fact she suffocated and died for a short period. After this operation, she could no longer talk, eat or drink and had a permanent naso- gastric tube draining her stomach. Indeed she never ate, drank or talked again.
It was decided that the area needed time to recover so nothing was done for a few months. Again kez was in and out with breathing problems until she had to have emergency surgery as the trachea which ws once pink and healthy, was dying and mutating. IT had developed a second blind branch into which her trachy tube kept falling suffocating her on almost a daily basis. The 7 hour emergency surgery helped her breathe once more so that a second transplant, this time using artificial tracheal tissue, could be performed in october 2011. The surgeons also hoped to remove the damaged oesophagus which was showing no signs of healing and replacing it with a section of large intestine”.
Keziah was left, on top of all the suffering, with permanent tracheostomy and the naso-gastric tube she feared and which she was promised by Macchiarini and O’Flynn she would certainly avoid thanks to their magic of regenerative medicine. The oesophagal fistula which Birchall described as “unrelated to the transplant” was first created by the intraoperative radiation therapy (IORT, details of this exact intervention: page 8, in Italian), administered by Macchiarini together with his guest O’Flynn, with Birchall’s explicit knowledge. The hole in the oesophagus was completely ripped open during a botched up UCLH intervention, which happened because the stent had to be reinserted. But why was the stent removed from Keziah’s airways in the first place? Not one survivor of cadaveric trachea transplants lived ever without a stent, including Birchall’s own patients Claudia Castillo and Ciaran Lynch. The dead cell-free trachea carcass collapses immediately or gets overgrown with scar tissue, which then suffocates the patient, this is why the graft must be kept open by a stent at all times. Why did Birchall and O’Flynn remove the stent anyway? To admire their miracle cure which never happened, and to harvest their fame?
Plastic trachea and death
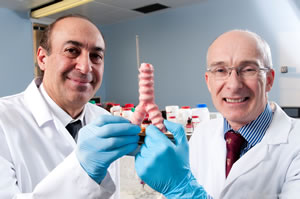
On September 29th 2011, as a palliative measure to extend Keziah’s life, Birchall implanted her with a plastic trachea, made at UCL and “regenerated” at Royal Free Hospital lab. Back then he seemed a big fan of those plastic tracheas. This is why UCL removed that photo of Birchall, where he holds a plastic trachea together with its maker, the UCL nanotechnologist Alexander Seifalian (who was sacked last year under a reason which Seifalian declared to me to be false and a pretence). The official version is that the transplant worked, but could not save Keziah due to previously incurred damage from a (non-existent) infection and oesophageal tear. Now we do know how lethal plastic tracheas are. Even Birchall knows. Why didn’t he ask Lowdell to make him another cadaveric one? Why didn’t he ask Elliott to procure one of his old-fashioned homografts (fixative-preserved cadaveric trachea) which worked well enough for Ciaran for 10 years? Because just some months before, first UCL-made plastic trachea was implanted by Macchiarini into his patient Andemariam Beyene at the Karolinska University Hospital in Sweden and declared a success. Which it of course was not.
Update 8.06.2017. Alexander Seifalian now told me his own version of what happened. According to this former UCL professor, Birchall pressured him to make a plastic trachea scaffold for Keziah. The UCL nanotechnology specialist didn’t want to, insisting that one needs to wait and see the outcome for Beyene. For whatever reasons, Macchiarini phoned Seifalian asking not to make this plastic trachea graft for Birchall. But the UCL laryngologist then engaged a joint PhD student of his and Seifalian’s to manufacture a plastic scaffold, which was declared to be intended for use as a stent. Birchall however then had that plastic scaffold “regenerated” by the Lowdell lab at Royal Free Hospital and implanted it as trachea replacement into Keziah.
Here the account from Keziah’s father on what happened next:
“The second transplant was a sucess and Kez had clear breathing for the first time in a year but the oesophagus repair could not take place, there was not enough undamaged tissue to stitch to so muscle from her neck was wrapped around the hole in the hope it would knit. It never did.
Over the next 2 months Kez had brief periods at home but there was soon signs that things were not right and bronchoscopy’s showed that scar tissue, where the new trachea was attached near her bronchi, was growing and again blocking off her airway. THis was lazered off but over the christmas period she developed pneumonia and she knew in herself that things were gettting difficult.
However noone expected that on the 9th january during a bronchoscopy, a specialist found that the tissue had grown so rapidly that Kez had less than 24 hours to live as the airway would be blocked off and this time there was nothing they could do. Kez was taken into an unconscious state with morphine and her life support was switched off at about 7am the next morning.
She was moved on her last day to a private room in intensive care where so many friends, relatives, and staff came to say their goodbyes to Kez. She managed to stay awake and smile to everybody on that last evening until she drifted into unconsciousness. When she was given the news, Kez was still insistant that she would fight on. Throughout the whole illness she believed she would win and be able to have a normal life with her ever loving boyfriend Joe who stood by her through everything.
Kez’s surgeon [O’Flynn, -LS] came to the funeral along with a number of the nurses who cared for her and even cleaning staff, all of whom had built their own relationships with Kez. Her surgeon spoke at her funeral. He also talked of her bravery and strength and selfless nature. He also talked of the invaluable knowledge gained by the research teams working on stem cell technology”.
Macchiarini in his usual manner could not be bothered about the patients he experimented upon. But Birchall sent a letter which was read out at Keziah’s funeral, appreciating her contribution to research. Which lessons did he draw from this human experiment of his though? Surprisingly, Birchall’s conclusion was that more patients need to be treated by this cadaveric trachea technology. As you can read here, here and here, phase I and phase II clinical trials are being prepared.

Donate!
If you are interested to support my work, you can leave here a small tip of $5. Or several of small tips, just increase the amount as you like (2x=€10; 5x=€25). Your generous patronage of my journalism will be most appreciated!
€5.00
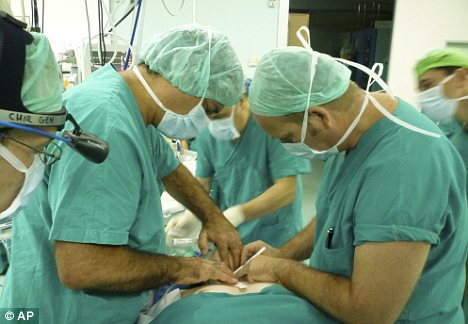

Are they are operating with bare hands?
LikeLike
It is obvious why UCL has gone silent about this. This is not simply a matter of a psychopathic con artist deceiving the doctors around him. Keziah’s family was not at all informed of the risks, the ethics board did not do basic checks, and the hospital assisted in covering up their failures for years after Keziah died. There appears to be sufficient proof of gross negligence and evil here to send people to prison.
LikeLike
The story at UCL looks similar to the story at Karolinska. Disastrous human experimentation followed by a cover-up. Have no-one spoken up against this at UCL like the doctors did at the Karolinska.
LikeLike
You just can’t get it right, can you Leonid? You are still misguided and inaccurate with your reporting on a number of counts. [Text removed, as breaching comment policy, -LS] I don’t even know why I bother to comment on here, but I guess I wouldn’t feel the need to if you did your research thoroughly enough to report the truth first time.
LikeLike
Dear tracehayter,
you allege inaccurate and dishonest reporting on a number of counts, but don’t provide any indication what the accurate account would be. Actually, nobody involved in this whole mess seems to be willing to shed light on what actually happened. The only undisputed fact seems to be that (almost) all involved patients are dead.
As an outsider, I find this behavior quite strange. Everybody stakeholder involved simply says the independent reporting in this blog is wrong – but without providing an alternative account that is at least internally consistent and matches up with what other participants have been claiming. This makes it very hard to sort out whose statements are clouded by “selfish ambition” (except for Macchiarini where this seems to be an established fact) and who is actually participating in destroying “the lives of others” (either for selfish ambition of scientific glory).
LikeLike
Pingback: Macchiarini’s trachea transplant patients: the full list – For Better Science
Pingback: Unpublished Macchiarini manuscript confirms 5 forgotten trachea transplant patients, Jungebluth’s surgery practice in Italy – For Better Science
Pingback: Berlin court grants Jungebluth new injunction against my reporting – For Better Science
Pingback: Alexander Seifalian, UCL’s Persian Scapegoat – For Better Science
Pingback: EU commemorates dead patients of Macchiarini & Birchall with a phase 2 trachea transplant trial TETRA – For Better Science
Pingback: Martin Birchall’s shaky road to mass trachea transplanting – For Better Science
Pingback: UCL fibs Parliament about trachea transplants – For Better Science
Pingback: Trachea transplanters: Round 2 at UK Parliament – For Better Science
Pingback: Birchall’s two dead pigs to prove trachea transplants are safe – For Better Science
Pingback: Trachea transplanters without borders – For Better Science
Pingback: UCL trachea transplant inquiry: scapegoating, obfuscation and a lost nose – For Better Science
Pingback: How Macchiarini was recruited to Karolinska – For Better Science
Telegraph 42 minutes ago: https://www.telegraph.co.uk/news/2018/10/30/scientists-behind-clinical-trial-accused-cover-deaths-two-young/
LikeLike
And this here: https://www.telegraph.co.uk/news/2018/10/30/ucl-researchers-lied-15-year-old-girls-transplant-disaster/
LikeLike
And this: https://www.telegraph.co.uk/news/2018/10/30/however-much-say-concerned-specific-patients-doctors-have-one/
LikeLike
Also here:
https://www.dailymail.co.uk/news/article-6335863/UCL-researchers-covered-deaths-two-young-women-controversial-stem-cell-treatment.html
LikeLike
Pingback: Paolo De Coppi and the UCL organ factory – For Better Science
Pingback: New government cash for trachea transplanters Videregen – For Better Science